WORKERS' COMPENSATION IN OKLAHOMA:
RECENT REFORMS AND RESULTS
Reforms enacted in recent years have centered on:
- Reducing health care costs through managed care.
- Requiring workplace safety programs.
- Creating a more politically independent judiciary.
- Strengthening fraud investigation and prosecution.
- Increasing the use of independent medical examiners.
- Making benefit payments more fair.
Legislative reforms have played a significant role in:
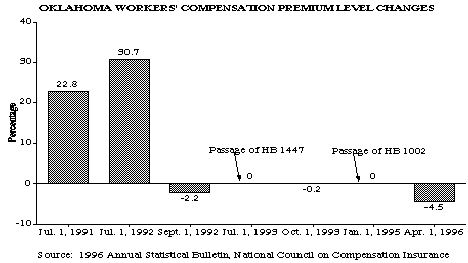
- Reducing workers' compensation costs by 4.5% in 1996 -- the largest reduction in a number of years.
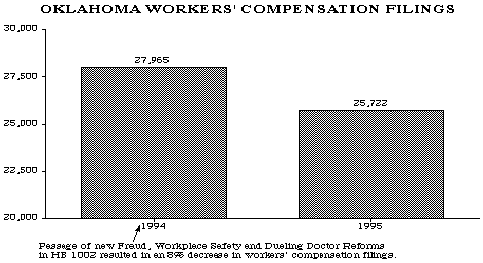
- Decreasing workers' compensation filings by 8% since 1994.
- Increasing the number of workers' compensation insurers writing policies in the state. Six new companies are writing policies since 1994.
- Covering more than 40,000 workers under nine new workplace medical plans. Five new plans have tentatively been approved by the State Insurance Fund.
- Increasing the number of fraud charges filed by 37% in the last year.
- Increasing the use of independent medical examiners in cases by 42% since 1995.
Reforms
In the past four years the Oklahoma legislature has enacted numerous reforms to the state's workers' compensation system. These reforms attempt to lower insurance costs to employers, control health care costs, improve work place safety and improve benefits and rehabilitation available to employees. Reforms have been enacted in nearly every area of workers' compensation but the most significant reforms have centered in 6 areas:
- Reducing Health Care Costs Through the Introduction of Managed Care;
- Requiring Workplace Safety Programs;
- Creating a More Politically Independent Judiciary;
- Strengthening Fraud Investigation and Prosecution;
- Increasing The Use of Independent Medical Examiners;
- Making Benefit Payments More Fair for Both Employers and Employees.
Results
Recent workers' compensation reforms have improved cost containment, workplace safety and lowered employers premiums in recent years. Some of the more significant results are:
- Legislative reforms have played a significant part in reducing workers' compensation costs according to the Oklahoma Insurance Department's Actuary. The Board of Property and Casualty Rates was presented with data in January of 1996 showing that enough savings have been achieved to warrant up to a 14% reduction in costs. The Board settled on a conservative 4.5% reduction in workers' compensation costs -- the largest reduction in a number of years. The actuarial study concluded that the real savings of many of the reforms would materialize in upcoming years.
- Stiffer fraud penalties, workplace safety, benefit changes and dueling doctor reforms have in part accounted for an 8% decrease in workers compensation filings since the reforms passed during a special session in 1994;
- Six new workers' compensation insurers are now writing policies in the state and workers' compensation lines are reported by some companies to be among their most profitable;
- More than 40,000 workers are now enrolled in workplace medical plans helping to further contain premium costs;
- Fraud charges have increased 37% in the last year with 92% of concluded cases ending in guilty pleas;
- The use of the Independent Medical Examiner in cases has increased 42% to date from when legislative changes were implemented in 1995;
- Enhancements to the workers' compensation counselor program designed to improve communication about the system to both employers and employees have had a significant impact in reducing unnecessary legal expenses to both employers and employees. The program has experienced a doubling of participation in educational seminars in 1996 and has saved Oklahoma employers hundreds of thousands of dollars in premium costs.
SPECIFIC REFORMS
Certified Workplace Medical Plan
The "certified workplace medical plan", a system of managed care which was established in 1994, allows employers to provide medical care to employees at a lower cost. Certified workplace medical plans provide medical care and payment for services on a fee-for-service basis to medical care providers and do not include capitated or prepaid plans. Currently, nine plans have been approved and one is pending approval.
Several of the plans have more than 10,000 enrollees, with at least two plans having more than 20,000 enrollees. Most plans have pending contracts with additional employers.
HB 2469, by Monson and Henry of the Senate and McCorkell of the House, allows any entity to organize a plan and make application to be a certified workplace medical plan. SB 1310, by Shedrick of the Senate and Steidley et al of the House, allows an insured employer to contract directly with a certified workplace medical plan if the insurer fails to contract with such a plan.
An insured employer with the State Insurance Fund may also contract directly with a plan, if the State Insurance Fund fails to contract with at least 3 plans, each covering at least 50 counties. The State Insurance Fund Board of Managers has tentatively approved five plans and will consider contracting with the plans during October of 1996.
Workers' Compensation Court
In 1992, in order to create a more politically independent judiciary, the Legislature required the names of reapplying incumbent judges to be sent directly to the Governor for reappointment. The time for trials and appeals in the Workers' Compensation Court has been reduced due to the expansion of the court to include a 10th judicial position in 1993 and the use of active retired judges, authorized by HB 1002 in 1994.
HB 1002 changed the name of the court's ombudsman program to the "Workers' Compensation Counselor" program and increased its duties. The counseling program provides information to employees and employers relating to the system which may decrease reliance upon private attorneys.
In 1995, new counselors responded to 21,000 requests for information and increased the number of written responses to employers and employees. More than 4,900 people were contacted through group presentations in 1995 and over 5,200 people have been reached through group presentations in the first nine months of 1996.
The program can point to a number of real success stories. For example, Holleytex, a carpet manufacturing plant in Watonga, saw its workers' compensation premiums drop by more than $400,000 from 1991 to 1995.
Compensability and Benefits
In 1992, the Legislature enacted a new definition of "injury" which requires heart-related injuries to result from excessive work-related stress, and prohibited the compensability of "mental only" claims by requiring that mental claims must be accompanied by a physical injury.
These reforms have resulted in an increase in denial of benefits. Also, since 1993, cumulative trauma injuries must meet a higher standard of proof, "preponderance of the evidence". This change will limit the compensability of injuries which occur over time and may be difficult to link directly to work.
Benefits were restructured in 1993 to establish a graduated, cumulative schedule of compensation with different numbers of weeks of award for different levels of impairment.
The effect of this change is to provide proportionately less benefits to less severely injured employees and more benefits to more severely injured employees. Also in 1993, vocational rehabilitation became mandatory before an award for permanent total disability could be ordered which will reduce the number of cases in which benefits are awarded. Death benefits were increased in 1994 to require higher payments for funeral expenses and increased lump sum benefits to surviving spouse and children. And, temporary total disability benefits were reduced by requiring the worker to ask the Court for an extension of benefits after only 42 weeks rather than the previous time period of 140 weeks.
This reduction in time prevents workers from receiving benefits after maximum medical improvement. In contrast, the maximum weekly benefit cap was increased from 75% to 90% of the state's average weekly wage in 1994 then to 100% in January of 1996. This will bring the cap closer to the national average.
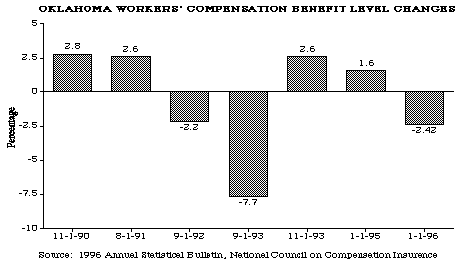
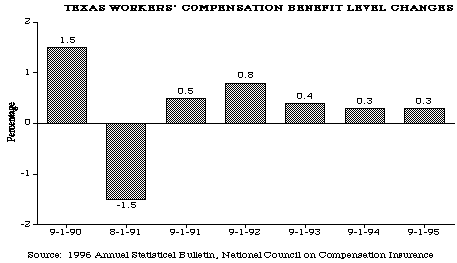
Fraud
The Workers' Compensation Fraud Unit was established in 1992 in the Attorney General's office for the investigation and prosecution of fraud. As the first single entity with this responsibility, the fraud unit has received more than 1200 complaints to date in 1996. Of these complaints, 94 charges have been brought against 51 defendants resulting in 33 guilty pleas, 16 cases pending, and 3 cases dismissed.
Since 1993, the fraud unit has been authorized by statute to impose additional criminal sanctions, examine additional records, and issue subpoenas. In 1994, the Legislature prohibited the use of "agents" or "runners" to solicit legal or medical business under the workers' compensation system.
Safety
In order to place a greater emphasis on worker safety, in 1993 the Legislature required every public employer with over 25 employees to develop a safety program. The State Department of Labor is responsible for the enforcement of this requirement along with an annual compilation of a list of the most hazardous industries for transmittal to insurers. Insurers must notify policyholders and make safety consultation services available. The 1996 list of most hazardous industries is currently available.
WORKERS' COMPENSATION - LEGISLATIVE HIGHLIGHTS
1992
- More politically independent judiciary created by requiring names of reapplying incumbent judges to be sent directly to the Governor for reappointment.
- Enactment of new definition of "injury" which requires heart-related injuries to result from excessive work-related stress. In 1991, 24% of orders for heart attack and stroke claims were denied benefits. By 1994, that number went up to 35%. This was a 45% increase in denial of benefits.
- Establishment of new method for calculation of average weekly wage (AWW) based on 5-day rather than 6-day work week.
- Prohibition of lump sum payments of attorneys fees in PTD cases.
- Establishment of Workers' Compensation Fraud Unit for the investigation and prosecution of fraud. AG's Fraud Unit had received 1260 complaints in July 1996. Ninety-four charges have been brought against 51 defendants resulting in 33 guilty pleas, 16 cases pending, and 3 cases dismissed.
1993
- Creation of the 10th judicial position on the Workers' Compensation Court which has allowed the court to set an additional estimated 7,000 cases a year.
- Benefits restructured to provide a graduated schedule of compensation based on the severity of the injury.
- Established the Physician Advisory Committee with authority to recommend improvements in the treatment and evaluation of work-related injuries.
- Creation of the "Certificate of Non-Coverage" for independent contractors who do not fall under the Workers' Compensation Act.
- Requirement for public employers with over 25 employees to develop a safety program.
1994
- Increase duties of ombudsman program and change of name to "Workers' Compensation Counselor" program. In 1995, new counselors responded to 30,000 requests for information and doubled the number of written responses to employers and employees. More than 4,900 people were contacted through group presentations in 1995. Over 5,100 people have been reached through group presentations in the first eight months of 1996 and over 15,000 requests for information have received responses.
- Change of time for compensability of injuries from 7 to 3 days.
- Prohibition of solicitation of workers' compensation claims by "agents" or "runners" from doctors or lawyers.
- Creation of new medical fee schedule to become effective on 1-1-96. NCCI estimates a 6.8% reduction in physician costs.
- Establishment of "certified workplace medical plan" which allows employers to provide medical care at lower costs. In 1995, two plans were approved. Currently, nine plans have been approved and one is pending. This is an increase of 350%.
- Establishment of the "independent medical examiner" (IME) system to create a list of qualified physicians to serve as IMEs. From 1995 to 1996, the use of IMEs increased by 42% with more than 4,600 IME exams scheduled in 1995. In the first six months of 1996, over 3100 IME exams have been ordered. By the end of 1996, this number should more than exceed the number of IME exams in 1995.
- Requirement for the State Department of Labor to compile a list of the most hazardous industries for insurers to use in identification of policyholders which may require safety consultation services. This list is currently available.
- Provided for the use of active retired judges on an as needed basis. Time for appeals has dropped from 10 to 8 weeks for TTD and from 19 to 12 weeks for PPD.
- Establishment of an alternative for workers' compensation coverage through an "equivalent insurance product."
 Oklahoma Senate
Oklahoma Senate

